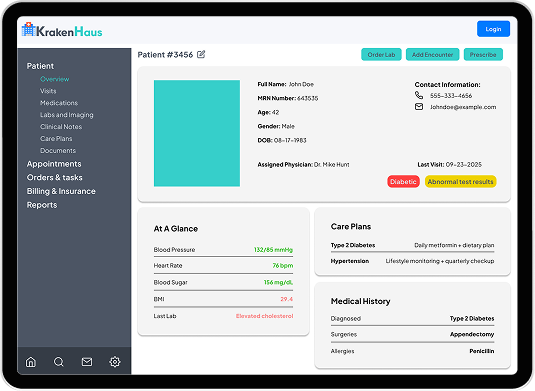
Healthcare providers deal with complex workflows, strict compliance requirements, and the constant need to improve patient care. Off-the-shelf EHR systems often lack the flexibility to adapt to unique operational needs, leaving gaps in efficiency and user satisfaction. Custom EHR software development bridges this gap, creating systems tailored to the way your practice actually works.
Why Organizations Choose Custom EHR Development
A well-designed EHR solution can be the difference between staff spending hours wrestling with the system or focusing on patient care. Custom development allows you to:
- Align with existing workflows so that staff do not need to adapt to rigid, generic processes.
- Integrate seamlessly with existing systems such as lab platforms, imaging software, billing tools, and telehealth solutions.
- Ensure compliance with regulations like HIPAA and ONC standards while maintaining security protocols tailored to your environment.
Key Components of a Custom EHR
Developing an EHR system involves more than just digitizing patient records. The right approach focuses on:
- Patient record management with easy access, search, and update capabilities.
- Interoperability features to exchange data securely with other healthcare systems.
- Scalable architecture to handle growing patient data and new features over time.
The Development Process in Action
A strong development process starts with understanding your clinical, administrative, and compliance priorities. Prototyping and iterative testing with actual end users ensure the final product is functional, intuitive, and reliable from day one.
Enhances operational efficiency, supports improved patient outcomes, and evolves alongside your organization.
For healthcare providers, every hour spent on manual paperwork, repetitive data entry, or fragmented workflows is an hour that could have been invested in patient care. Administrative tasks consume valuable resources, increase operational costs, and can slow revenue cycles. Purpose-built EHR software development offers a direct route to eliminating these inefficiencies, enabling faster decision-making, improved accuracy, and measurable financial returns
Eliminating Redundant Workflows
Many healthcare organizations still rely on multiple systems that do not communicate well with each other. Staff must enter the same information in different places, increasing the chance of errors and duplications. Custom-built EHR and EMR software can unify these touchpoints, automatically populating patient data across modules such as scheduling, billing, and clinical records. This reduces staff workload and prevents revenue loss caused by incomplete or inconsistent records.
Impact on ROI: Less time spent on repetitive work allows staff to handle more patient interactions without increasing headcount, directly improving productivity and profitability.
Streamlining Documentation and Compliance
Regulatory documentation is a major source of administrative burden. A well-designed EHR software development solution can incorporate automated coding assistance, pre-configured compliance templates, and built-in validation checks. This ensures that every patient encounter is documented accurately, supporting faster claims submission and reducing the risk of denials.
Impact on ROI: Cleaner claims and fewer resubmissions shorten the revenue cycle and minimize lost income from compliance errors.
Enhancing Interdepartmental Coordination
Disjointed communication between departments can create delays, whether in processing lab results, managing referrals, or updating patient histories. An integrated EHR system centralizes all relevant information, making it instantly accessible to authorized users across departments. This improves care coordination and eliminates time-consuming back-and-forth communication.
Impact on ROI: Faster information flow reduces patient wait times, increases throughput, and improves patient satisfaction scores — which can translate into higher reimbursements.
Supporting Data-Driven Decision Making
Custom EHR development can embed advanced analytics that track operational metrics in real time. From identifying bottlenecks in patient check-in to spotting billing slowdowns, these insights help healthcare leaders act quickly to resolve inefficiencies.
Impact on ROI: Data transparency empowers leadership to make operational improvements that yield cost savings and long-term revenue growth.
The Strategic Value
While the upfront investment in EHR software development can be significant, the payback is tangible. Lower administrative overhead, improved cash flow from faster reimbursements, and increased staff capacity to focus on patient care all contribute to measurable ROI. For CXOs and CTOs, the real benefit lies in transforming the EHR from a record-keeping tool into a central operational asset that drives both efficiency and profitability.
For a senior leader, investing in custom EHR software is a strategic decision that impacts operational efficiency, compliance, patient outcomes, and long-term scalability. Choosing
the right development partner requires looking beyond surface-level promises and evaluating their ability to deliver solutions that align with organizational goals.
Proven Healthcare Domain Expertise
A partner must demonstrate a deep understanding of healthcare workflows, regulatory frameworks, and interoperability standards. This includes practical experience with HIPAA, ONC guidelines, and clinical data exchange protocols such as FHIR and HL7. A vendor familiar with payer, provider, and pharmacy systems can anticipate integration challenges and design solutions that work seamlessly across the care continuum.
Customization That Reflects Real-World Needs
Off-the-shelf solutions rarely fit every department or specialty. A capable EHR development partner will invest time in understanding existing workflows, identifying inefficiencies, and designing features that improve clinical efficiency. This may include specialty-specific templates, role-based dashboards, or streamlined order entry to reduce clicks and improve documentation speed.
Interoperability and Integration Capabilities
An EHR cannot exist in isolation. The right partner ensures that the system integrates smoothly with other healthcare applications such as lab systems, imaging tools, telehealth platforms, and billing software. Their approach should include robust APIs, secure data exchange mechanisms, and testing for both inbound and outbound data flows.
Scalability and Future-Proof Architecture
Healthcare organizations evolve rapidly, and so should their EHR. A strong partner builds scalable architecture capable of supporting new features, increased user loads, and emerging technologies such as AI-powered decision support. Cloud-based deployments with modular components allow upgrades without disrupting ongoing operations.
Focus on User Experience
Adoption depends heavily on usability. Senior leaders should expect a partner who conducts thorough user research and designs interfaces that minimize cognitive load for clinicians and staff. Intuitive navigation, quick access to patient data, and mobile responsiveness are no longer optional; they are essential to productivity and satisfaction.
Security and Compliance as a Priority
Data breaches can damage both finances and reputation. A qualified development partner embeds security from the outset, with encryption in transit and at rest, multi-factor authentication, detailed audit trails, and continuous monitoring for vulnerabilities. Compliance with HIPAA and other relevant regulations must be built into the development lifecycle, not treated as an afterthought.
Transparent Communication and Project Management
Clear milestones, documented progress, and open lines of communication are critical for project success. Senior leaders should look for partners who provide regular updates, involve stakeholders in decision-making, and have a defined process for handling change requests without scope creep.
A successful EHR go-live is less about a single launch day and more about how well the development partner anticipates and neutralizes risks from the start. Senior leaders know that any disruption during implementation can erode confidence among clinicians and slow ROI.
Structured Pilot Sprints to Validate Real-World Performance
Leading EHR developers begin with focused pilot sprints, deploying the system to a small group of users in a controlled environment. This approach helps identify integration issues, workflow mismatches, and performance gaps before full-scale rollout. Feedback from these pilots shapes refinements that prevent larger-scale failures.
Staging Environments for Safe Testing
A top-tier EHR software development company uses staging environments that mirror the production system. This allows teams to test configurations, updates, and data migrations without touching live patient records. It also enables clinicians and administrators to explore new features in a safe space before they go live.
Clinician-Centric Training
Effective training strategies focus on role-specific workflows. Developers work with internal trainers to create scenario-based learning modules that reflect actual daily tasks. This shortens the learning curve and ensures clinicians are ready to work efficiently on day one.
Hypercare Support After Go-Live
A smooth launch is reinforced by hyper care, a period of intensive post-go-live support where developers and IT teams are on standby to resolve issues immediately. By combining real-time troubleshooting with proactive monitoring, the development partner ensures that early adoption challenges are resolved before they can affect patient care or productivity.
An off-the-shelf EHR may appear cost-effective at first, but many healthcare organizations discover hidden costs when workflows, compliance requirements, or specialty-specific needs do not align with a generic system. For leaders making long-term technology investments, the difference between a poor fit and a tailored solution can shape operational efficiency for years.
Precision Fit for Complex Workflows
Custom EHR software solutions are built to match the exact processes of the organization. From patient intake to billing, every screen and automation is designed around the way staff already work, reducing the time spent adapting to rigid templates.
Flexibility to Evolve with the Organization
A reputable EHR/EMR software development company creates systems with scalability in mind. As regulations change or service lines expand, new modules and integrations can be added without replacing the core system. This adaptability ensures technology investments remain viable over the long term.
Competitive Advantage Through Data and Insights
Tailored systems give healthcare providers better control over how data is captured, analyzed, and visualized. Leaders can access performance dashboards, predictive
analytics, and specialty-specific reports that off-the-shelf tools cannot deliver without heavy customization costs.
Reduced Risk of Vendor Lock-In
With a custom build, the healthcare organization owns its system roadmap. This prevents reliance on a single vendor’s release cycle, pricing model, or product limitations, enabling more control over cost and innovation pace.
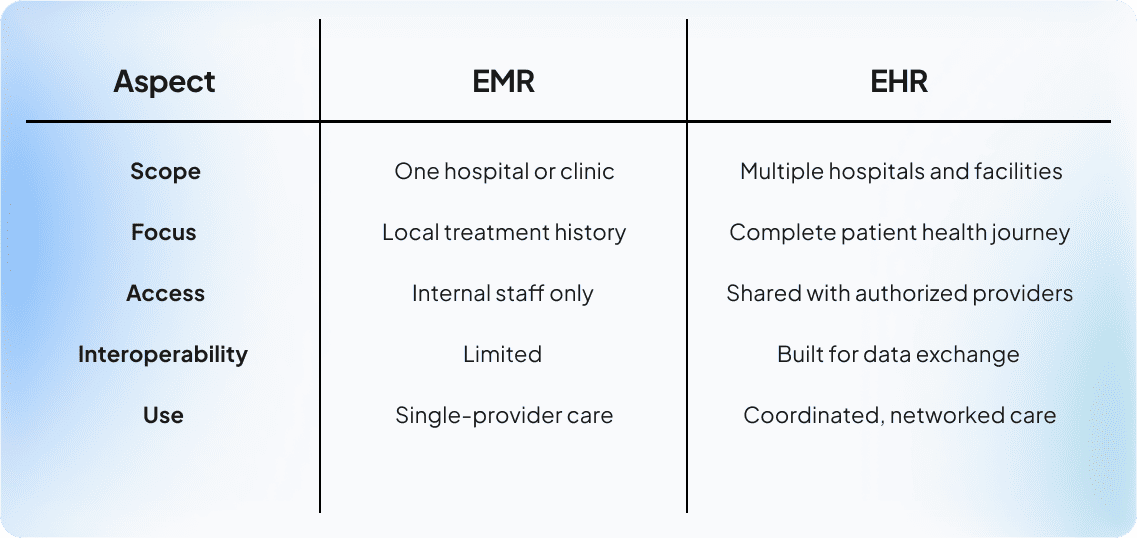
For healthcare providers, the right Electronic Health Record (EHR) or Electronic Medical Record (EMR) system isn’t just about digitizing patient charts—it’s about transforming how clinical, operational, and administrative teams work together. When implemented effectively, these solutions deliver measurable improvements in patient outcomes, compliance, and organizational efficiency.
Improved Patient Care and Safety
EHR/EMR systems centralize patient histories, lab results, medication lists, and imaging data, making critical information available in real time. Clinicians can make better-informed decisions, avoid duplicate tests, and flag potential drug interactions before prescribing.
Key Outcomes:
- Faster access to complete medical histories
- Reduced clinical errors through decision support alerts
- More personalized treatment planning
Streamlined Workflows and Efficiency
Paper-based processes create bottlenecks in scheduling, billing, and care coordination. EHR/EMR platforms automate repetitive tasks like appointment reminders, insurance verification, and coding.
Key Outcomes:
- Reduced administrative burden for staff
- Quicker patient check-ins and discharges
- Higher throughput without compromising quality of care
Enhanced Compliance and Reporting
Modern EHR solutions are designed with HIPAA, NIST, and other regulatory frameworks in mind. Built-in audit trails, encryption, and secure access controls safeguard patient data while simplifying compliance reporting.
Key Outcomes:
- Automated audit logs for every data access or change
- Simplified preparation for compliance audits
- Stronger data security posture
Interoperability and Data Sharing
Integration with labs, pharmacies, imaging centers, and other healthcare providers ensures data flows seamlessly across the care continuum. Standards like HL7 and FHIR enable interoperability that supports better collaboration.
Key Outcomes:
- Faster test result sharing between providers
- Reduced patient data silos
- Improved care coordination for chronic and complex cases
Financial and Operational Gains
EHR/EMR adoption can reduce costly errors, shorten billing cycles, and improve revenue capture through accurate coding and claims submission.
Key Outcomes:
- Higher first-pass claims approval rates
- Less revenue lost to denied claims
- Better financial forecasting through integrated analytics
Data-Driven Decision Making
With built-in analytics and reporting, healthcare leaders can track key performance indicators (KPIs), identify trends, and make proactive changes to care delivery models.
Key Outcomes:
- Real-time dashboards for operational visibility
- Predictive insights into patient populations
- Evidence-based strategy planning